|
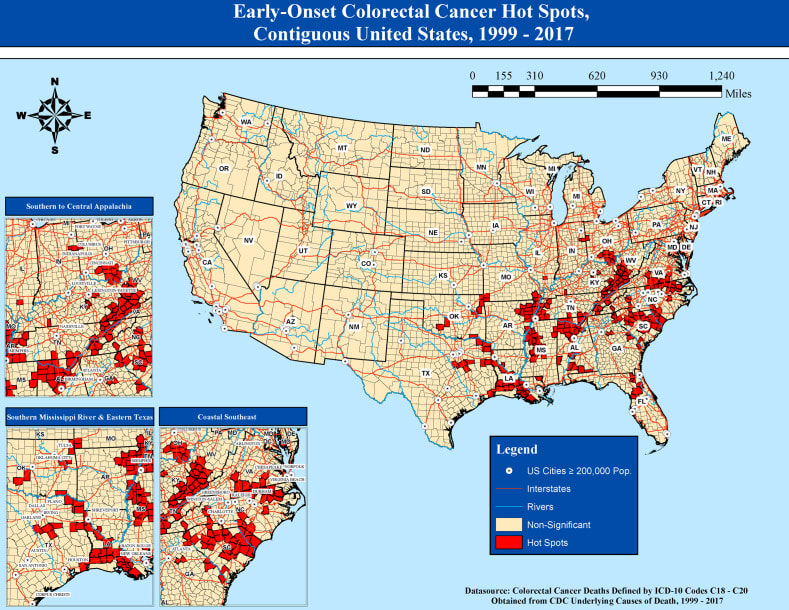
When the news dropped of Chadwick Boseman’s death at the age of 43, I, like so many others, was in complete shock. Such an amazing talent couldn’t be gone so soon, it just didn’t make any sense. He was a game-changing actor, rising at a seemingly unstoppable rate to great heights in his career. His role as “Black Panther” revolutionized the superhero movie genre and Chadwick himself came to embody unmatched strength, power, and courage. Little did we know that he was even more courageous than we could ever imagine, as he’d spent years privately battling colon cancer. Chadwick’s death rocked us to our core. Like the deaths of many of those who were taken seemingly before their time, it was almost impossible to wrap our heads around. He was just too young. For Black Millennials in particular, it was a sobering moment to contend with. Even in the face of other possible threats to our lives, we were forced like never before to come face to face with our own mortality. Because if the man who so convincingly embodied a superhero could be taken so soon by sickness, then we’re all fair game. The cold, hard truth is that colorectal cancer rates are rising among people of younger ages. While we’ve grown to understand colorectal cancer as something that hits people in their fifties, sixties, or older, more and more Millennials, who are currently in their thirties and forties, are experiencing an uptick in cases. While it still remains relatively rare, the rate of colorectal cancer in adults under 50 has doubled since 1990. Such an increase in such a short amount of time can’t be attributed to genetics, and is more than likely being caused by environmental factors such as poor diet, lack of exercise, smoking, and possible environmental toxicants. Boseman was born and raised in Anderson County, South Carolina, which is one of 232 counties in the United States that have been identified as a hotspot for early-onset colorectal cancer. The majority of these hotspots are located in the Southern U.S., with other counties located further up on the East coast. In these hotspots, survival rates are significantly worse among Black men. This also suggests that the root cause is environmental rather than genetic. This isn’t the only racial disparity that exists for Black people when it comes to colorectal cancer. Blacks are more likely to develop and die from colorectal cancer at a young age than Whites in general, and it may have a lot to do with the environments that we’re raised in. While the common refrain is that we simply don’t know what’s causing this uptick in cases, there’s a lot that is known that points to a necessary need for increased vigilance amongst Black Americans.
The Diet Switch Study In 2015, a study was conducted comparing the diets of African Americans with rural South Africans. While colon cancer is the second leading cause of cancer death among Western nations, it’s actually relatively rare among rural Africans. The study sought to find out if diet was the cause. The initial screening of the gut microbiome of both groups found biomarkers of increased cancer risk among the Black Americans, such as more polyps and higher levels of potentially pathogenic bacteria. In the guts of the rural Africans, signs of anti-inflammatory, anti-neoplastic (anti-tumor) byproducts of fiber fermentation were found. The diets of both groups were then switched, with the rural Africans eating a more Westernized, high-fat diet while the Americans ate the more high-fiber, low-fat diet of the rural Africans. Within just two weeks, the rural Africans developed colonic inflammation and signs of increased colon cancer risk. The Americans’ diet change showed a decrease of the biomarkers that indicated increased colon cancer risk. One biomarker, secondary bile salts, which is a known carcinogen, was reduced by 70% in the American group after switching to a rural African diet. For the rural Africans, their secondary bile salts shot up by 400% eating a typical Western diet. To put it simply, eating a rural African diet made the American guts healthier while eating a standard American diet gave the rural Africans an increased risk of developing disease. This one study illuminates what a lot of us already instinctively know. The high-fat, low-fiber Standard American Diet is damaging to our health, and drastically increases the risk of developing colon cancer. An earlier study in 1999 suggested that it isn’t simply the lack of fiber that explains the differences in colon cancer rates between Black Americans and rural Africans, but the presence of “aggressive” factors such as too much animal protein and high-fat meals, as well as differences in bacterial fermentation in the gut. Another study found that there is indeed a difference in the bacterial population in the guts of African Americans even when compared to Whites in the U.S. African Americans tend to have a higher population of Bilophila wadsworthia, an inflammatory bacteria linked to cancer growth. This type of bacteria proliferates when fed a diet high in fat and animal protein. The Right Way To Feed Yourself - And Your Gut Bacteria There are certain things we know when it comes to the development of colon cancer. Red and processed meats have been found in a number of studies to be linked to an increased risk of colon cancer. High intake of ultra-processed foods has also been linked to colon cancer, with smokers being especially susceptible. Being overweight or obese also increases the risk of developing colon cancer, especially for men and especially if the weight is gained starting in early adulthood. Taking everything into account, one thing becomes clear: how we eat matters. Eating a diet rich in red and processed meats as well as high fat foods while neglecting to eat fiber-rich, antioxidant-rich, anti-inflammatory foods on a regular basis sets us up for poor health outcomes and dramatically increases our risk of developing a number of life-threatening diseases, including colon cancer. When we eat, we aren’t simply feeding ourselves. We’re also feeding the trillions of tiny bacteria that live in our gut. There are many different kinds of gut bacteria, each of which thrive depending on the environment of our gut. The bacteria that imparts a protective effect on our health thrive on a variety of fiber-rich plant foods while the bacteria that promote inflammation and cancer growth thrive on high-fat foods. Unfortunately, the way we’ve been taught to eat creates a disease-causing environment in our gut. The good news is, if the diet switch study is any indication, our gut microbiome can change simply by changing our diets. Removing red, processed, and high-fat meats from the diet is the biggest change that you can make right now. Adding in beans, seeds, whole grains, and other forms of plant protein can help build up the populations of protective bacteria in your gut. Eat a variety of fruits and vegetables to reap the benefits of a multitude of health-promoting phytonutrients. Finally, get up and move! Your gut motility, the movement of food through your gut, is influenced by your body’s movement. This may be one reason why lack of physical activity is linked to increased colon cancer risk. The Need For Course Correction When I think of Millennials being diagnosed with and succumbing to colon cancer at a young age, I can’t help but think back to my childhood and teenage years. It was completely normal for my peers and I to eat processed meat on a daily basis in some form. Bacon, egg & cheese sandwiches, pepperoni pizzas, deli meat sandwiches, hot dogs, canned corned beef and vienna sausages were among the many high-fat, processed-meat based meals that I ate both at home and served to me at school. I definitely did not consume enough vegetables, fruits, beans, or whole grains, all of which contain nutrients that help to protect against disease. Imagine spending your most formative years, when your body is growing and developing, eating a diet full of foods that increase your risk of colon cancer and other chronic diseases. Imagine doing that for many years, from elementary school through high school, and beyond. After two or three decades, we’ve cultivated a gut that is ripe for disease. Even without smoking, even with leading an active lifestyle (which I personally didn’t), it would only be a matter of time before it all caught up. Let me be clear: we didn't choose this. We did not choose to be born into a society where our only nutrition education came from TV and billboard advertisements. We didn't choose to be born into communities without adequate access to fresh produce. We didn't choose to be born into neighborhoods overrun with fast food spots and liquor joints. We grew up in unhealthy environments shaped by forces beyond our control and quite often beyond the control of our parents. We grew to adopt eating habits and behaviors that served corporate interests without any real knowledge of just how much damage it was doing to our bodies. But now that we're old enough to make our own choices, we have to be honest with ourselves about the lifestyles we've come to embrace, even if they weren't our choices to begin with. We’re the hot dogs at every game, circus, or movie generation. We’re the meat lovers, pile it all on, stacks of processed meat on our pizza generation. We’re the bacon on every. damn. thing generation. We’re the cheese in the crust, cheese in every possible thing you can put it in generation. We’re the deep fry anything that can survive a vat of hot oil generation. We’re the watch TV, play video games, chill on our phone instead of going outside to play generation. We were raised on a lifestyle that has brought us here: a doubling in the rate of colon cancer over the course of a single generation - ours. Now that we’re aging, we’re seeing the effects of our younger years catching up to us. The good news is, there’s something that can be done about this. We just have to be willing to take an honest look at our lifestyles and have the courage to reject the unhealthy foods and habits that we were raised upon. Adopting a plant-based, active lifestyle changed my life and improved my health dramatically. While I may not know what the future brings or how much damage might have been done in the first couple decades of my life, I know that I can do what’s in my power now to ensure that I don’t keep making the same mistakes. For Black people, poor people, and those of us raised in food deserts and food swamps, a change in lifestyle is absolutely urgent. Colon cancer is just one of many preventable lifestyle-based diseases that plague our communities, taking away our loved ones well before their time. If the past year and a half has taught us anything, it’s that taking control of our health is absolutely paramount, even while we’re “young”.
1 Comment
7/1/2024 08:35:20 am
I wanted to express my gratitude for your insightful and engaging article. Your writing is clear and easy to follow, and I appreciated the way you presented your ideas in a thoughtful and organized manner. Your analysis was both thought-provoking and well-researched, and I enjoyed the real-life examples you used to illustrate your points. Your article has provided me with a fresh perspective on the subject matter and has inspired me to think more deeply about this topic.
Reply
Leave a Reply. |
AuthorMy name is Nivea, but you can call me Niv. I'm an independent Plant-Based Nutrition & Fitness Coach hailing from the Bronx, NY. Archives
August 2021
Categories
All
|



 RSS Feed
RSS Feed